|
Until 2000, pneumococcal infections caused 60,000 cases of invasive disease such as meningitis and pneumonia each year. An “invasive” disease means that germs invade parts of the body that are normally free from germs. When this happens, disease is usually very severe, requiring treatment in a hospital and in some cases causing death. You have probably heard of pneumonia, which is an infection of the lungs. Pneumonia can be caused by many different bacteria, viruses, and even fungi, but pneumococcus is one of the most common causes of severe pneumonia. Many bacteria, including some Streptococcus pneumoniae (pneumococcus), have become resistant to one or many antibiotics. Available data also show that up to 40% of these infections were caused by pneumococcal bacteria that were resistant to at least one antibiotic. However, with the introduction of pneumococcal conjugate vaccines for children (PCV7 and PCV13), cases of invasive pneumococcal disease dropped to approximately 34,000 in 2013, and resistance rates have reduced to 30%.
This demonstrates that PCV7 and PCV13 are preventing infections caused by drug-resistant pneumococcal strains. Not only have morbidity and mortality rates decreased, costs associated with the infection have plummeted as well. These higher costs were because of the need for more expensive antibiotics; repeat disease due to treatment failures; the need for surveillance to track resistance patterns; educational requirements for patients, physicians, and microbiologists; and new antibiotic drug development. The pneumococcal conjugate vaccine (PCV13 or Prevnar 13®) protects against the 13 types of pneumococcal bacteria that cause most of the severe illness in children and adults. The vaccine can also help prevent some ear infections. PCV13 is recommended for all children at 2, 4, and 6 months, and again at 12-15 months old. PCV13 is also recommended for adults 19 years or older with certain medical conditions and in all adults 65 years or older. By getting vaccinated, you can help Nevada reduce its rate of pneumococcal infections, and curb the increasing rate of antibiotic resistance. For more information, visit: http://www.cdc.gov/pneumococcal/about/infection-types.html http://www.cdc.gov/pneumococcal/drug-resistance.html
0 Comments
Get Smart About Antibiotics Week is an annual observance to raise awareness of antibiotic resistance and the importance of appropriate antibiotic prescription and use. The principle of antibiotic resistance is that over time bacteria evolve to resist the drugs we take to fight them. This means an antibiotic that works against a certain bacteria today might not work in the future, so we need to be careful about antibiotic prescribing.
Antibiotics are among the most commonly prescribed drugs used in human medicine, and up to 50% of all the antibiotics prescribed for people are not needed or are not optimally effective as prescribed. Because of this, the use of antibiotics is the single most important factor in driving adverse antibiotic resistance rates around the world. Unfortunately, each year in the United States, at least 2 million people become infected with bacteria that are resistant to antibiotics, and at least 23,000 people die as a direct result of these infections. Of particular concern here in Nevada is the bacterium Clostridium difficile, which has symptoms ranging from diarrhea to life-threatening inflammation of the colon. Recent trends over the years have shown an increase in the rate of hospitalizations, and are expected to continue to rise. To address this issue, on Sept. 18, 2014, the White House announced an Executive Order stating that the federal government will work domestically and internationally to detect, prevent, and control illness and death related to antibiotic-resistant infections by implementing measures that reduce the emergence and spread of antibiotic-resistant bacteria and help ensure the continued availability of effective therapeutics for the treatment of bacterial infections. In light of this nationally recognized observance week, the Nevada Antimicrobial Stewardship Program has partnered with physician organizations, consumer groups, health plans, state and local public health organizations and pharmaceutical companies to educate health professionals and consumers about the appropriate use of antibiotics. Through these collaborative efforts, the goal is to increase awareness about the overuse and misuse of antibiotics, and prevent the increase and spread of antibiotic-resistant bacteria among all Nevada residents. To learn more, please visit our Antibiotic Resistance Page here. Every year around this time, we start hearing mumbles and grumbles about flu season. The flu season is unpredictable; it varies from year to year and in different parts of the country. However, a good rule of thumb for flu season is October through May.
Getting the flu vaccine The flu vaccine can prevent you from getting the flu, make flu symptoms less severe if you are exposed, and prevent you from spreading the flu to others. The Centers for Disease Control and Prevention (CDC) recommends the flu vaccine for everyone 6 months of age and older. It’s best to get vaccinated as soon as the vaccine becomes available in your area so as many people as possible are vaccinated by the time flu season really kicks off. If you are lagging on getting your vaccine and find yourself in the middle of flu season with no protection, it’s not too late! As long as the flu virus is still circulating in the community, it’s not too late to get vaccinated. Visit https://influencenevada.org/healthcare-providers/ or http://flushot.healthmap.org/ to find the most convenient location for you and your loved one to receive your flu vaccine. One of the main reasons people say they didn’t get the flu vaccine is that they got it before and still got sick. There are a few reasons this could happen:
But will the flu vaccine itself make me sick? No, a flu vaccine cannot cause illness because it does not contain any live virus. Those who do experience slight side effects might feel soreness at the injection site, hoarseness, red or itchy eyes, cough, fever, aches, headache, itching, or fatigue. This could be mistaken for flu-like symptoms, but will be minor and short in duration (one to two days). After I’ve gotten the flu vaccine, what extra steps can I take to protect myself? Stay away from sick people, wash your hands, and avoid touching your eyes, nose or mouth. It’s important to practice other healthy habits such as cleaning and disinfecting frequently touched surfaces at home and work (door handles, phones, hand rails, sinks, etc.). Also get plenty of sleep, stay active, manage the stress in your life in a healthy way, drink plenty of fluids, and eat nutritious food. What if I do get the flu? If you are infected, there are antiviral drugs that can be used to treat the flu. Those at high risk for complications (children younger than 2, adults older than 65, pregnant women, and people with certain medical conditions) and people who are very sick with the flu (such as those who are in the hospital due to their illness) should get antiviral drugs. It’s important to remember that antibiotics won’t work against the flu. Antibiotics are useful against bacteria but not viruses. It’s also important to stay away from others if you are sick so you don’t spread the virus, so please don’t go to work or school if you have the flu. For the 2016-2017 flu season, the CDC’s Advisory Committee on Immunization Practices (ACIP) recommends the nasal spray vaccine not be used. Only injectable flu vaccines are recommended for this season. Millions of people get sick, hundreds of thousands are hospitalized, and thousands or even tens of thousands die from the flu every year in the United States — so take the easy step of protecting yourself by getting vaccinated!
The Behavioral Risk Factor Surveillance System (BRFSS) is a telephone survey that collects state-level data about people who live in the United States. It began with 15 states in 1984, which makes it the longest-running survey system in the world, but has spread to all 50 states, the District of Columbia, and three U.S. territories and conducts more than 400,000 adult interviews each year. This valuable tool tells us a lot about health risk behaviors at the state and local levels, helps target and build health promotion and disease prevention programs, and helps to guide legislative efforts in each state.
This valuable survey asks U.S. residents about their health-related risk behaviors and efforts, chronic health conditions, and use of preventive services. It also addresses important emerging health issues such as vaccine shortage and influenza-like illness. Each state uses a standardized rotating core questionnaire and optional modules are available. States are also able to add their own questions according to their needs. The rotating core questionnaire is available on the Centers for Disease Control and Prevention (CDC) website at http://www.cdc.gov/brfss/questionnaires/index.htm. The rotating core is comprised of two different sets of questions that are asked in alternating years by all states. In the years that rotating core topics are not used, they are offered as optional modules. Adults 18 years or older are asked to take part in the BRFSS. Respondents are not compensated for their time, but they should know they are doing their part in helping to improve the health of people in their state and the nation. Until 2011, the survey was conducted via land lines using random digit dialing, but with the decrease in homes that have land lines the survey was expanded to include cell phones. Many different agencies sponsor the BRFSS. For example, most divisions within the CDC sponsor this important survey, as well as federal agencies such as the Health Resources and Services Administration, Administration on Aging, Department of Veterans Affairs, and Substance Abuse and Mental Health Services Administration. Other countries are catching on to the utility of the BRFSS and have requested technical assistance from the BRFSS staff. These countries are Australia, Brazil, Canada, China, Egypt, Italy, Jordan, South Korea, Mexico, nations in the Caribbean, and Vietnam. The BRFSS in Nevada Nevada’s Chronic Disease Prevention and Health Promotion (CDPHP) Section’s overall goal is to improve quality of life and extend years of healthy living and the BRFSS has been an important source for monitoring health-related factors and evaluating the success of programs. The survey data are used to set program goals and monitor progress at the state and local levels in Nevada. In general, the BRFSS provides data for the CDPHP section to:
More specifically, the CDPHP uses BRFSS data to monitor and compare a program’s target populations in terms of their health conditions (cardiovascular disease, hypertension, high blood cholesterol levels, diabetes, overweight, obesity, and disability), risk factors (smoking, alcohol use, insufficient physical activity, and insufficient fruit/vegetable consumption), preventive services use (blood cholesterol checks, mammograms and Pap tests for women 40 years or older, colorectal cancer screening in individuals 50 years or older, and dental checkups), and access to health care (measured as any coverage of health insurance). In Nevada, we also use the BRFSS data to:
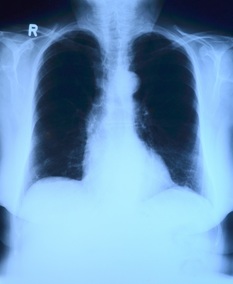
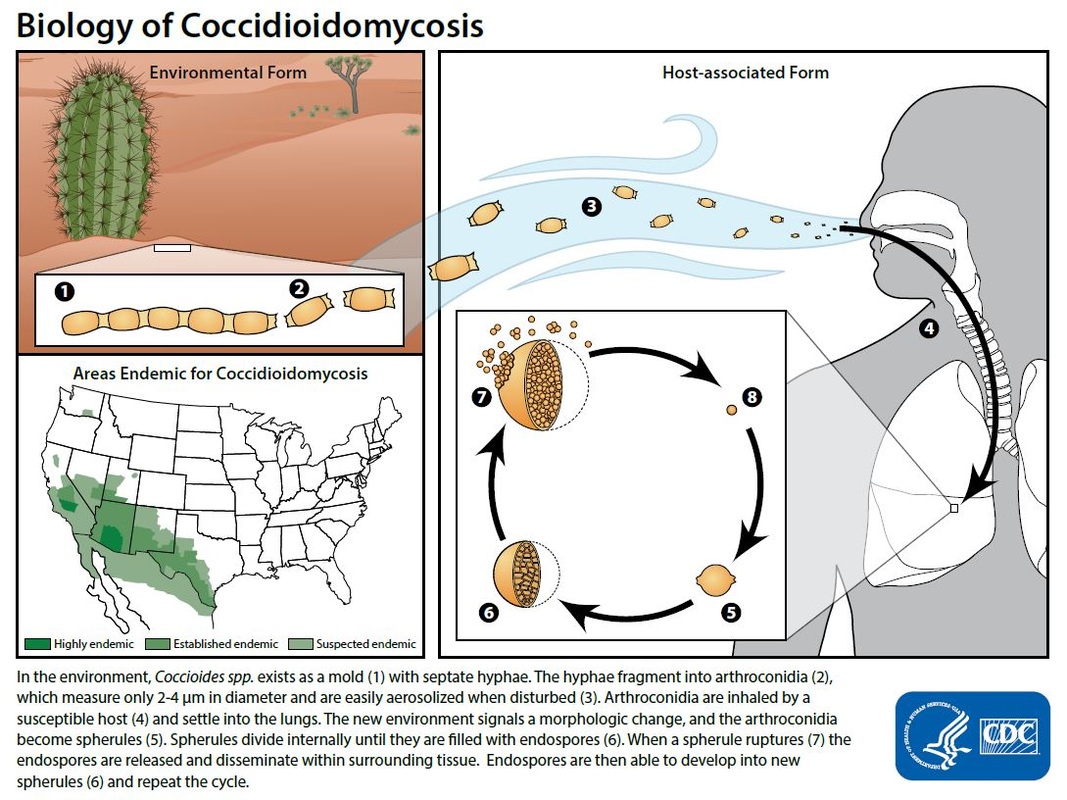
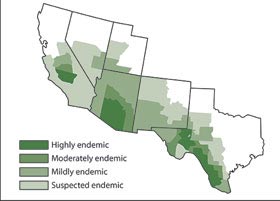
Want to know how Nevada compares on important health indicators? Find out CDC’s handy widget below! Valley Fever is an infection with symptoms similar to pneumonia: fatigue, cough, fever, shortness of breath, headache, night sweats, muscle aches or joint pain, and a rash on the upper body or legs. It is caused by a fungus that lives in the soil and has been found in Nevada. So far this year, there have been 33 cases in Clark County and 4 in Washoe County. This can be explained by the fact that Clark County is more populated than Washoe County, and it’s also in the southern part of the state where the fungus that causes Valley Fever is endemic. Coccidioidomycosis is caused by the fungus Coccidioides, which is known to live in the soil in the southwestern United States (Arizona, California, Nevada, New Mexico, Texas, or Utah) and parts of Mexico, Central and South America. The fungus was also recently found as far north as south-central Washington State. People can get Valley fever by breathing in the microscopic fungal spores from the air, although most people who breathe in the spores don't get sick. Valley Fever can affect people of any age, but it's most common in adults aged 60 and older. Other groups of people may be at higher risk for developing the severe forms of Valley Fever are:
It is very difficult to avoid breathing in the fungus that causes Valley Fever in areas where it's common in the environment. People who live in these areas should try to avoid spending time in dusty places. The following are some common-sense methods to help avoid getting Valley Fever. Although these steps are recommended, they haven't been proven to prevent Valley Fever:
There is no vaccine for Valley Fever at this time, but scientists have been trying to make one since the 1960s. For more information about Valley Fever visit: http://www.cdc.gov/fungal/diseases/coccidioidomycosis/index.html When it comes to HIV, the term “new diagnoses” does not always mean a new infection. According to the Centers for Disease Control and Prevention (CDC), approximately 45,000 people were newly diagnosed with Human Immunodeficiency Virus (HIV) in 2014. Thirty percent of those new HIV infections were transmitted by people living undiagnosed. The CDC estimates that more than 1.2 million people are living with HIV, and more than 150,000 HIV-positive individuals were living undiagnosed between the years of 2005 and 2014. The number of new HIV diagnoses in the United States has decreased 19%, but not all regional or demographic groups are affected equally. While national improvements in HIV testing and surveillance practices have resulted in an overall decrease of new cases between 2005 and 2014, between 2006 and 2015 in Nevada the number of new HIV diagnoses has increased 16% due to the improvements in testing and surveillance.
In 2015, there were 477 new HIV diagnoses statewide, which is a 14% increase from the 420 new HIV diagnoses in 2014. The number of new cases has remained stable between 2014 and 2015 in all counties in Nevada with the exception of Clark County. In 2015, youths age 15 to 25 have experienced a slight decline in new cases but there have been increases in those age 25 to 54. The greatest increase in 2015 has been in the 35- to 44-year-old group, showing an increase of 46%. Looking at these numbers, it’s important to remember that many of these new cases have been diagnosed due to a national shift towards targeted testing and increased surveillance services. In the ‘80s and ‘90s, HIV was considered a terminal condition where many who were infected typically did not expect to live much longer than a few years after diagnosis. Fast forward 30 years, HIV has become a chronic disease where those infected can prevent transmission to non-HIV-positive partners via Pre-Exposure Prophylaxis (PrEP), have non-HIV-positive children, and experience many years of life while in care. In Nevada at the end of 2015, a total of 10,138 persons were known to be living with HIV, including more than half (52%) having been diagnosed with Acquired Immune Deficiency Syndrome (AIDS). Overall, the rate of new HIV diagnoses, new AIDS cases, and deaths among persons living with HIV/AIDS, has been steadily declining. Fewer people are becoming infected and people are living longer once they do become infected. Although many advances have been made in HIV/AIDS treatment, prevention and care, geographic, gender, age, and racial/ethnic disparities still exist within our state. The best prevention is knowledge. Thirty percent of all new HIV cases nationally are being transmitted from those who are undiagnosed. Everyone should know their HIV status, especially those who engage in higher risk behaviors such as injection drug use, men who have sex with men, and sex with anonymous partners. Knowing is the first step in the right direction to diminish the number of new HIV diagnoses into the future. Check out OPHIE’s HIV/AIDS Surveillance program at http://bit.do/OPHIEHIV. CDC- HIV Basic Statistics- http://www.cdc.gov/hiv/basics/statistics.html Acute flaccid myelitis (AFM) is a condition that affects the nervous system, specifically the spinal cord. Most people who experience AFM will have limb weakness, but some people also experience facial droop/weakness, difficulty moving the eyes, drooping eyelids, and difficulty swallowing or slurred speech. Numbness or tingling is rare, and some people experience pain in their arms and legs. Severe symptoms include respiratory failure as a result of breathing muscles that become weak. AFM has no specific treatment, but interventions may be ordered by a doctor on a case-by-case basis.
AFM has a variety of causes, but viral infections such as enteroviruses (polio and non-polio), West Nile Virus (and viruses in the same family), herpes viruses, and adenoviruses have been attributed to the cause of AFM. You can prevent AFM by staying up to date on all recommended vaccinations, including poliovirus. You can also protect yourself and your family from mosquito-borne viruses that can cause AFM by using mosquito repellent and staying indoors at dawn and dusk. Other ways you can protect yourself from causes of AFM (and, let’s face it, other gross things) are:
Gov. Brian Sandoval proclaimed May 2-6, 2016, as Nevada Employee Appreciation Week. In his proclamation, Gov. Sandoval stated that Nevada’s state employees are truly deserving of appreciation, respect, and gratitude for the professionalism and commitment with which they carry out their mission.
As a way to celebrate the hard work we do for Nevadans, the Office of Public Health Informatics and Epidemiology (OPHIE) and other Division of Public and Behavioral Health staff participated in themed days throughout the week: Monday: represent your favorite cause, such as a charity or raising awareness Tuesday: wear a jersey or your t-shirt to support your favorite sports team or college Wednesday: wear tennis shoes or show off the silliest pair of shoes you own Thursday: show off your favorite band or artist by wearing their t-shirt Friday: dress for your favorite holiday We had a blast showing off our favorite duds, check us out below! The local chapter of the American Statistical Association (ASA) hosted a Spring Social on Friday, April 29, 2016. Two of our OPHIE Biostatisticians, Chief Biostatistician Kyra Morgan and Facility Biostatistician Yucui Liu, are members of the local ASA chapter; the chapter’s objectives are to promote statistics and its applications and to increase the contributions of statistics to human welfare. Part of the Spring Social included a talk given by Dr. Javier Rojo, the Chair of the Department of Mathematics and Statistics at the University of Nevada, Reno. Dr. Rojo discussed the history of statistics and highlighted many contributors to the field. It’s a little known fact that the field of statistics is relatively young, but it is growing rapidly.
Because the field is so young, Dr. Rojo was able to study under many of the big names in statistics, including his advisor being Erich Lehmann. Erich Lehmann studied directly under Jerzy Neyman who has made many famous contributions to the field, such as the Neyman-Pearson Lemma. The Neyman-Pearson Lemma plays a large role in the field of hypothesis testing. OPHIE’s Chief Biostatistician, Kyra Morgan, was able to take one of the most fundamental statistics courses from Dr. Rojo. |
AuthorOPHIE records and analyzes data from disease investigations, identifies risk factors, and provides education on disease prevention in Nevada. Archives
November 2018
Categories |









 RSS Feed
RSS Feed
