|
Buckle up buttercups, we are getting personal this month and talking about what goes on behind closed doors… bathroom doors that is. Around 48 million people in the U.S. get sick every year from food-borne illness. Common symptoms of food-borne illness include an upset stomach, stomach cramps, nausea, vomiting, diarrhea, and fever. During the holiday season, it is especially important to be mindful of food-borne illness when large amounts of food are being prepared and served to family and friends. What causes food-borne illness?
There are many different bacteria, viruses, and parasites that can contaminate food causing food-borne illness. This month, we are going to highlight two commonly known bacteria (Salmonella and E. Coli) and one that you may be unaware of (Bacillus Cereus). Salmonella is a bacterium that can infect both humans and animals. You can become infected by eating contaminated raw or under cooked food – especially:
Next up is E. coli, a bacterium that normally live in the intestines of healthy people and animals. You can be infected by eating contaminated water or food- especially:
Lastly, the bacterium you may be unaware of that can infect your holiday food is Bacillus Cereus. Bacillus Cereus is a spore-forming bacterium that can grow at a variety of temperatures in a short amount of time. This emetic syndrome (nausea/vomiting) is usually associated with starchy foods such as:
From our OPHIE family to yours, have a happy and food safe Thanksgiving!
128 Comments
This month we are bringing awareness to cancer, being that it is also Breast Cancer Awareness month! Here are the Nevada OPHIE office we have a team of people dedicated to the data collection of cancer through the Nevada Central Cancer Registry (NCCR). The purpose of this program is to use the data to evaluate the appropriateness of measures for the prevention and control of cancer in Nevada. There is a lot of misinformation on the Internet these days, so it is our hope to share a few key facts about cancer and how you can take some steps in prevention and early detection. How can I protect against and prevent cancer myself?
Some cancers, such as skin cancer, can be prevented with protective measures. Even though summer is coming to an end, don't put away that sunscreen. Out on the mountain slopes while snowboarding, skiing, or sledding it is important to put sunscreen on exposed skin such as your face. UV rays can reflect up from the snow adding to the UV coming down directly above you. Being at an increased altitude also plays a factor into the likelihood of burning while shreddin the gnar.
Breast cancer and testicular cancers are two cancers that you can try to detect early on your own. Women of all ages are encouraged to perform self-exams at least once a month to be familiar with how your breasts look and feel so that you can alert a health care professional if there are any changes. It's important to note that men can also get breast cancer as well. More than 200,000 cases of breast cancer occur in the United States every year. In the shower, in front of a mirror, or lying down, using the pads of your fingers, move from the outside to the center, examining the entire breast feeling for lumps, thickening of tissue, or hardened knots. Testicular cancer is the most common form of cancer in men ages 15-35. Every year in the United States, more than 9,000 men are diagnosed with testicular cancer. Self-examination is crucial and should be performed at least monthly so that if you notice a change, you can contact a health care professional for further examination. For men, preferably standing in front of a mirror if possible, check both testicles for swelling. Additionally, examine the testicles with your thumb and fingers noticing for any irregularities on the surface or tissue. Did you know that West Nile Virus is the most commonly spread pathogen by mosquitos in the continental United States? In fact, there were over 2,000 cases of West Nile Virus reported to the Centers for Disease Control and Prevention (CDC) last year. How can I protect myself?
Although cases differ from year to year and state to state, all 48 continental United States have reported cases since 1999. In the United States, cases are reported through summer and into fall. Washoe County Health District confirmed on July 25, 2018 that mosquito samples from the Damonte Ranch area and Hidden Valley Areas have tested positive for West Nile Virus. What is my risk? Although everyone is at risk for West Nile Virus, some people are at increased risk for severe disease, which includes the brain and spinal cord. For example, those over the age of 60 are at higher risk for encephalitis (swelling of the brain). What are the symptoms of West Nile Virus?
What can I do to control mosquitos?
The hot summer months are in full swing, and that means you need to take extra precautions to stay safe. Did you know there are several different illnesses related to heat? Heat Stroke is the most serious heat related illness. It happens when the body is not able to control its temperature: the body’s temperature rises rapidly, the sweating mechanism fails, and the body is unable to cool down. When heat stroke occurs, the body temperature can rise to 106°F or higher within 10 to 15 minutes. Death or permanent disability can occur if the person does not receive emergency treatment. Symptoms
Heat Exhaustion is the body’s response to the excessive loss of water and salt. This usually happens though sweating. The elderly, those with high blood pressure, and those who are working in a hot environment are most prone to heat exhaustion. Symptoms
Rhabdomyolysis is a medical condition associated with heat stress and prolonged physical exertion, resulting in the rapid breakdown, rupture, and death of muscle. When muscle tissue dies, electrolytes and large proteins are released into the bloodstream that can cause irregular heart rhythms and seizures, and damage the kidneys. Symptoms
Heat syncope is a fainting episode or dizziness that usually occurs with prolonged standing or sudden rising from a sitting or lying position. Factors that may contribute to heat syncope include dehydration and not being acclimated to your surroundings. Symptoms
Heat cramps usually affect people who sweat a lot during strenuous activity. This sweating depletes the body’s salt and moisture levels. Low salt levels in muscles causes painful cramps. Heat cramps may also be a symptom of heat exhaustion. Symptoms
Heat rash is a skin irritation caused by excessive sweating during hot, humid weather.
Symptoms
Beat the heat by drinking plenty of water! Be sure to check in on friends and neighbors who are at high risk for heat related illness. People who are at high risk are infants, young children, older adults, and people with chronic medical conditions. Seek air conditioning (this is a great excuse to go to the mall or the library!). NEVER leave kids or pets in the car, even for a minute. If you go outside remember to limit your time outdoors, and bring a hat, sunscreen (SPF 15 or higher), water, and lightweight and light colored clothing. Also, don’t forget your pets this time of year! Our furry friends are susceptible to heat related illness too, so check out these tips from the ASPCA on how to keep your pets safe. The time is here for summer cookouts and picnics! That means lots of fun with friends and family, but it also means opportunity for foodborne illness. But why? Temperatures tend to be warmer, and these gatherings sometimes occur away from clean running water and refrigeration. But you can still keep your food safe to eat by using an insulated cooler. You can use ice, gel packs, or even frozen food to keep your food cold, and remember to minimize opening and closing the cooler so your food stays colder longer. Also keep in mind that a cooler full of cold food will stay colder longer than a partially full one. Finally, remember to keep the cooler out of the direct sun by placing it in the shade or another shelter. Keep cold food cold and hot foods hot. Cold perishable food should be kept in the cooler at 40 °F or below until serving time.
Hot food should be kept hot, at or above 140 °F.
When grilling, be sure to prepare foods using separate cutting boards for raw meat and ready to eat foods like fruit and vegetables. Be sure to use a clean plate and a clean set of tongs for serving cooked food, this way you don’t reuse items that have touched raw meat. Use a meat thermometer to ensure your food has reached safe internal temperatures: When eating outside, be sure to never let food sit out for longer than two hours, and if the temperature is over 90 °F do not let food sit out for longer than one hour. Also, bacteria tend to multiply faster when it’s warm, so choose to serve cold food in smaller portions and keep the rest in the cooler. Remember these four simple steps to safe food handling.
CLEAN Wash hands and surfaces often
Separate raw meats from other foods
Cook to the right temperature
Refrigerate foods promptly
Now that you’ve been reminded of basic food safety, get out there and enjoy your summer BBQs! What is CRE? CRE, which means Carbapenem-resistant Enterobacteriaceae, are a family of over 70 different germs that have high levels of resistance to antibiotics which makes them difficult to treat. While Enterobacteriaceae are part of the normal human gut flora, Klebsiella species and Escherichia coli (E. coli) for example, these gut bacteria can develop resistance to antibiotics and become a dangerous infection. The way these bacteria develop their resistance to antibiotics is they create enzymes, called carbapenemase, to neutralize carbapenems and make them ineffective. Carbapenems are often considered the last line of defense against serious infections. Another way CRE can become resistant to carbapenems is through the production of beta-lactamases, an enzyme that neutralizes a different kind of antibiotic called beta-lactam, in combination with changes to the bacteria’s cell membrane. Who is at risk for getting a CRE infection? Healthy people are not at risk for CRE infections. The infections usually occur in people who are in hospitals, nursing homes, and other healthcare settings. Those who utilize devices, such as ventilators, intravenous or urinary catheters, and those who are taking long courses of specific antibiotics are most at risk for CRE infection. CRE infections typically happen among sick patients who are receiving treatment for another condition. What is the difference between infection and colonization?
CRE can be responsible for either colonization or an infection. Colonization means that there are CRE in or on someone’s body, but it’s not causing any symptoms. Colonization can progress to cause infections if they gain access to the right part of the body. That is why those who use devices are at high risk; those devices provide a portal for the CRE to start an infection. Colonized people are also capable of spreading CRE to others. What can I do to prevent a CRE infection? CRE is usually spread person to person through contact with infected or colonized people, particularly contact with wounds or stool.
What are hospitals doing to prevent CRE infections?
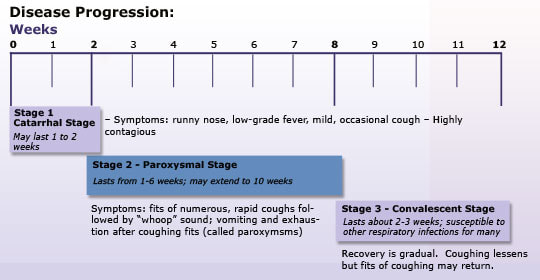
How is CRE treated? This infection is often resistant to many of the common antibiotics, but they may still succumb to one or more other antibiotics. People who are colonized with CRE do not require any treatment. Pertussis, also known as whooping cough, is a respiratory illness caused by a bacteria that attaches itself to the upper respiratory system. These bacteria release toxins that damage the tiny, hair-like extensions that help keep the airway clean, and causes the airway to swell. The bacteria is very contagious, and only found in humans. It spreads by an infected person coughing or sneezing or when they spend a lot of time sharing breathing space with others. Babies who get pertussis are usually infected by older siblings, their parents, or their caregivers who may not even know they are carrying the disease. They are at high risk for complications from pertussis, but death from whooping cough is rare. But, while it is rare, it can still happen. Read Jazzlyn’s story here. The Details The time between being infected and showing symptoms of pertussis is 7 to 10 days, but can range from 4 to 21 days. The three stages of pertussis are outlined below: Treatment Treatment recommendations for pertussis are antibiotics, however the guidelines aren’t so simple. It is recommended that persons older than 1 year of age be treated within 3 weeks of cough onset, and infants younger than 1 year of age and pregnant women (especially who are near their due date) within 6 weeks of cough onset. However, the Centers for Disease Control and Prevention (CDC) promotes the appropriate use of antibiotics among health care professionals and patients. The CDC recommends targeting postexposure antibiotic treatment at people at high risk for developing a severe case of pertussis. Prevention The pertussis vaccine is the most effective way to prevent the disease. It’s important to remember that no vaccine is 100% effective, but if someone has gotten the vaccine and they still get sick the infection is usually milder. One way mothers can protect their babies is to get a Tdap vaccine (which covers tetanus, diphtheria, and pertussis) during the third trimester of each pregnancy. The recommended time to get the vaccine is the 27th through 36th week of pregnancy, and the earlier during this time period the better. The mother’s body is able to pass on protective antibodies to the baby even before it is born. Babies are then able to receive their own immunization starting at 2 months of age. You may have heard of a Tdap vaccine and a Dtap vaccine. These are essentially the same vaccine; they both protect against tetanus, diphtheria, and pertussis. Dtap is for those younger than 7 years of age, and Tdap is for those who are 7 years old or more. What is norovirus? You may have heard people talk about the “stomach flu,” but there’s no flu that causes gastrointestinal symptoms; what they really mean is norovirus. As its name describes, norovirus is a virus that is highly contagious and it can infect someone more than once in your life. You build no immunity to it. Anyone can become infected with norovirus at any time, but the most common months for infection in the United States are November through April. What are the symptoms of norovirus?
Symptoms usually develop 12-48 hours after being exposed to the virus, and the illness usually goes away within 1-3 days. Because the illness causes vomiting and diarrhea multiple times a day it can cause dehydration, especially in young children, older adults, and people with other illnesses. If dehydration occurs, you will notice a decrease in urination, a dry mouth and throat, and a feeling of dizziness. Children who are dehydrated may cry with few or no tears, and may be unusually sleepy or fussy. How would I get norovirus? Norovirus is the leading cause of illness and outbreaks from contaminated food sources in the United States. Most outbreaks begin in food service settings when ill food service workers touch ready to eat items (such as raw fruits or vegetables) with their bare hands. However, any food that is served raw or is handled after being cooked can be contaminated with norovirus. Outbreaks also can occur when foods are contaminated at their source, such as oysters, fruits, and vegetables. When am I most contagious? You are most contagious when you are sick with the virus, and during the first few days after you recover from the illness. But how do I get norovirus in the first place? Gross alert! You become infected with norovirus by accidently ingesting stool or vomit from someone else who is infected. This can happen by consuming food or liquids that are contaminated with the virus, touching a surface that has norovirus on it and then putting your fingers in your mouth, or having contact with someone who is infected with norovirus (for example, sharing food or eating utensils with someone who has norovirus). For this reason, norovirus can quickly spread through closed places like daycare centers, nursing homes, schools, and cruise ships. Sounds gross. What do I do to protect myself?? Basic tips:
All these steps sound easy, but what do I do if I get sick anyway?
There is no specific treatment for norovirus; and because it is a virus, antibiotics do no good. If you do get norovirus, or any other gastrointestinal illness, be sure to drink plenty of liquids. Sports drinks or other drinks with no caffeine or alcohol can help with mild dehydration, but oral rehydration solutions are more helpful and you can get them over the counter. If you think you or someone you are caring for is severely dehydrated, call the doctor. It’s turkey month! Many of us are looking forward to Thanksgiving dinner later this month, but it’s important to remember food safety during this time. The Centers for Disease Control and Prevention (CDC) estimates that every year about a million people get sick from eating poultry contaminated with harmful germs. To avoid getting sick, it’s important to take steps to protect your health and the health of those for whom you are cooking. In the store:
Once Thanksgiving dinner is done, it’s important to still keep food safety in mind. Be sure to refrigerate leftovers within two hours to prevent bacteria from growing on food. Use shallow pans or containers to store leftovers; this decreases the time it takes for food to leave the unsafe temperature zone where bacteria can grow (40˚F to 140˚F). Remove leftover stuffing from inside your turkey and store it separately. And, while we all love Thanksgiving leftovers, it’s best not to consume leftovers after they have been in the refrigerator for more than 3-4 days (this means the Tuesday after Thanksgiving). Use the freezer to store leftovers for longer periods of time. Need some fun recipe ideas to help use up those Thanksgiving leftovers before they go bad? Check out this blog for yummy recipes! Pregnant at Thanksgiving? Take these extra precautions! Skip the eggnog, it can contain raw eggs and unpasteurized milk which can carry Salmonella. Also pass on the unpasteurized apple cider, there’s a danger of E. coli. Both of these can cause severe gastrointestinal symptoms and high fever, which put you and your pregnancy at risk. Best to just stick to other beverages. Although they are so yummy, avoid soft cheeses and cold cuts. Soft cheeses like brie, camembert, blue cheese, and cheeses made with unpasteurized milk can cause illness, as can cold cuts. If cold cuts cannot be avoided, be sure to heat to steaming hot or to a minimum temperature of 165˚F. Flu Season is Here! Every year around this time, we start hearing mumbles and grumbles about flu season. The flu season is unpredictable; it varies from year to year and in different parts of the country. However, a good rule of thumb for flu season is October through May. Getting the flu vaccine The flu vaccine can prevent you from getting the flu, make flu symptoms less severe if you are exposed, and prevent you from spreading the flu to others. The Centers for Disease Control and Prevention (CDC) recommends the flu vaccine for everyone 6 months of age and older who do not have contraindications. It’s best to get vaccinated as soon as the vaccine becomes available in your area so as many people as possible are vaccinated by the time flu season really kicks off. If you are lagging on getting your vaccine and find yourself in the middle of flu season with no protection, it’s not too late! As long as the flu virus is still circulating in the community, it’s not too late to get vaccinated. Visit https://influencenevada.org/healthcare-providers/ or http://flushot.healthmap.org/ to find the most convenient location for you and your loved one to receive your flu vaccine. One of the main reasons people say they didn’t get the flu vaccine is that they got it before and still got sick. There are a few reasons this could happen:
But will the flu vaccine itself make me sick? No, a flu vaccine cannot cause illness because it does not contain any live virus. Those who do experience slight side effects might feel soreness at the injection site, hoarseness, red or itchy eyes, cough, fever, aches, headache, itching, or fatigue. This could be mistaken for flu-like symptoms, but will be minor and short in duration (one to two days). After I’ve gotten the flu vaccine, what extra steps can I take to protect myself? Stay away from sick people, wash your hands, and avoid touching your eyes, nose or mouth. It’s important to practice other healthy habits such as cleaning and disinfecting frequently touched surfaces at home and work (door handles, phones, hand rails, sinks, etc.). Also get plenty of sleep, stay active, manage the stress in your life in a healthy way, drink plenty of fluids, and eat nutritious food. What if I do get the flu?
If you are infected, there are antiviral drugs that can be used to treat the flu. Those at high risk for complications (children younger than 2, adults older than 65, pregnant women, and people with certain medical conditions) and people who are very sick with the flu (such as those who are in the hospital due to their illness) should get antiviral drugs. It’s important to remember that antibiotics won’t work against the flu. Antibiotics are useful against bacteria but not viruses. It’s also important to stay away from others if you are sick so you don’t spread the virus, so please don’t go to work or school if you have the flu. For the 2017-2018 flu season, the CDC’s Advisory Committee on Immunization Practices (ACIP) recommends the nasal spray vaccine not be used. Only injectable flu vaccines are recommended for this season. Millions of people get sick, hundreds of thousands are hospitalized, and thousands or even tens of thousands die from the flu every year in the United States — so take the easy step of protecting yourself by getting vaccinated! |
AuthorOPHIE records and analyzes data from disease investigations, identifies risk factors, and provides education on disease prevention in Nevada. Archives
November 2018
Categories |


















 RSS Feed
RSS Feed
