|
The nation is witnessing a growing number of people addicted to opioids, which has exacerbated the issue of unsafe injection practices among injection drug users. In addition to the dangers of drug use itself, injections can be unsafe when needles and syringes are shared. Diseases can be spread this way. For example, if someone who has hepatitis C or HIV uses injection equipment on themselves and then shares it, any subsequent users of that injection equipment are then exposed to the disease. That person may then share their equipment, and the cycle begins again. This is where syringe services programs come in. Among many other services, these programs offer sterile injection equipment and collection/disposal of used injection equipment. This removes the need for sharing because new equipment is available to everyone at no cost. It also removes used equipment from the community and helps to decrease the risk of accidental exposure. This protects the community, law enforcement, first responders, among many others. Syringe services programs operate under the harm reduction model. This model uses practical strategies and ideas aimed at reducing negative consequences associated with drug use. It follows several principles. It:
There are currently two syringe services programs in Nevada. Northern Nevada HOPES houses Change Point, Nevada’s first syringe services program. The second syringe services program, Trac-B, is located in Las Vegas; this program is the first in the nation to offer syringe vending machines. People who want to use these machines need to register first with the program to receive a swipe card and unique ID number, then they can use their card to receive up to two kits per week. These machines are located at several locations around Las Vegas:
If you or someone you know needs these services, contact:
Change Point 445 Ralston St. Reno, NV 89503 Phone: (775) 997-7519 Email: [email protected] Hours: Monday – Friday 9:00am – 5:00pm Trac-B Exchange 6114 W. Charleston Blvd. Las Vegas, NV 89146 Phone: (702) 840-6693 Email: [email protected] Hours: Monday 1:00pm – 6:00pm Tuesday 10:00am – 2:00pm Wednesday 10:00am – 2:00pm Thursday 10:00am – 2:00pm Friday 9:00am – 12:00pm HIV and HCV testing every Wednesday during business hours.
4 Comments
Hand hygiene is critical to avoid getting sick and spreading germs to others all year round. Handwashing serves as a DIY vaccine against diarrheal and respiratory illness.
When should you wash your hands?
How should you wash your hands?
It’s important to remember, the space under your fingernail can harbor bacteria as well so be sure to wash under your fingernails. It’s recommended that health care providers wear natural fingernails with tips less than a quarter inch long. What if you don’t have access to soap and clean, running water? If soap and water are not available, use an alcohol based hand sanitizer that contains at least 60% alcohol. Keep in mind while sanitizers can reduce the number of germs in some situations, they do not remove all germs and might not remove harmful chemicals. How do you use hand sanitizers?
What about C. diff? Hand sanitizers are not effective against C. diff, so if you have it or are caring for or visiting someone with C. diff be sure to wash your hands with soap and water. Be sure to check out OPHIE’s Hand Hygiene training! It’s worth .5 CEU’s! The time is here for summer cookouts and picnics! That means lots of fun with friends and family, but it also means opportunity for foodborne illness. But why? Temperatures tend to be warmer, and these gatherings sometimes occur away from clean running water and refrigeration. But you can still keep your food safe to eat by using an insulated cooler. You can use ice, gel packs, or even frozen food to keep your food cold, and remember to minimize opening and closing the cooler so your food stays colder longer. Also keep in mind that a cooler full of cold food will stay colder longer than a partially full one. Finally, remember to keep the cooler out of the direct sun by placing it in the shade or another shelter. When grilling, be sure to prepare foods using separate cutting boards for raw meat and ready to eat foods like fruit and vegetables. Be sure to use a clean plate and a clean set of tongs for serving cooked food, this way you don’t reuse items that have touched raw meat. Use a meat thermometer to ensure your food has reached safe internal temperatures: When eating outside, be sure to never let food sit out for longer than two hours, and if the temperature is over 90 °F do not let food sit out for longer than one hour. Also, bacteria tend to multiply faster when it’s warm, so choose to serve cold food in smaller portions and keep the rest in the cooler.
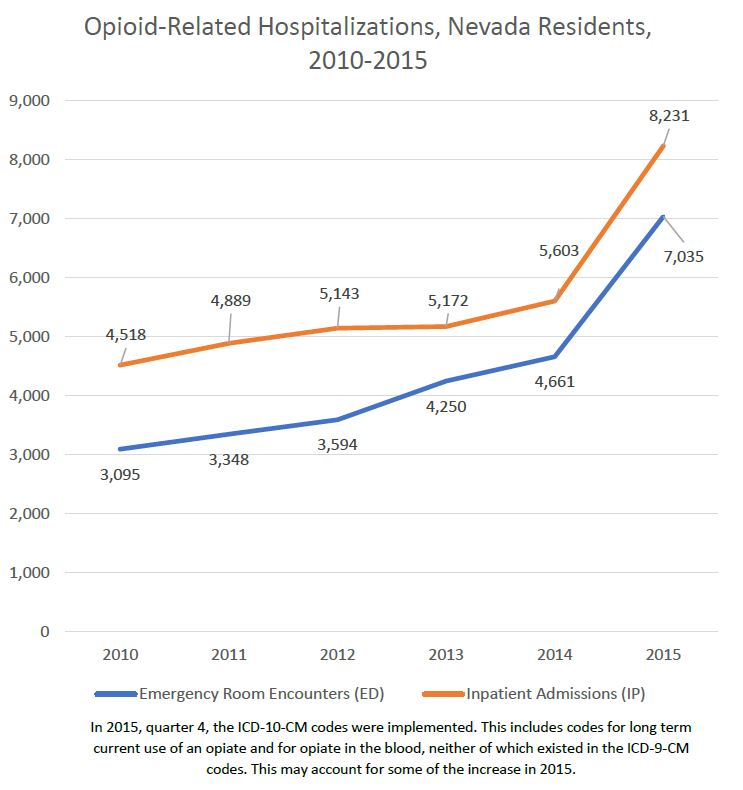
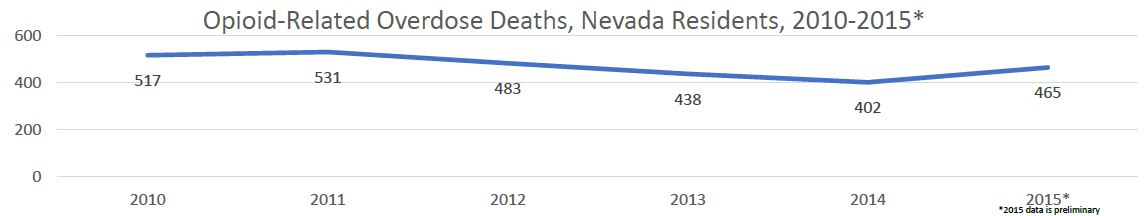
Now that you’ve been reminded of basic food safety, get out there and enjoy your summer BBQs! All recommendations from: https://www.foodsafety.gov/keep/events/summervacations/index.html It’s no secret that opioid use is on the rise nationwide. In fact, more than 60% of overdose deaths involve an opioid, and since 1999 the number of overdose deaths involving opioids have quadrupled. When people think of opioids they typically think of heroin, but they often forget about opiates prescribed for pain by a health care provider. In fact, overdoses from prescription opioids are a major contributor to the 15 year increase in overdose deaths in the United States. Nevada is no exception to the increase in opioid use. Between 2010 and 2015, Emergency Room encounters related to opioids more than doubled, and inpatient admissions increased by nearly 75%. Opioid related hospitalizations do not discriminate against one particular age range; in 2015, over a quarter of Emergency Room encounters and over a third of inpatient admissions were among patients aged 55 and over. Opioid-related overdose deaths in Nevada have decreased by 15% between 2010 and 2015, and the greatest number of deaths each year occur among those who are 45-54 years of age. Prevention is key in decreasing, and ultimately eliminating, overdose deaths. Prevention can take many different forms: education, stewardship of opioid prescriptions, and overdose reversal drugs such as naloxone. In fact, naloxone was administered to almost 15% of Emergency Department patients with opioid poisoning in Nevada in 2015. Naloxone is an opiate antagonist that can reverse the effects of an opioid if administered in time; it binds to the opiate receptors in the brain, taking the place of an opioid. Nevada recently codified into the Nevada Revised Statutes (NRS) the Good Samaritan Drug Overdose Act, provides protections to those who call for help in the case of an overdose, and it also expands access to naloxone. At this time, CVS and Walgreens locations in Nevada stock naloxone.
People receiving medical care can catch serious infections called healthcare associated infections (HAIs). One type of HAI – caused by the bacteria Clostridium difficile – was estimated to cause almost half a million infections in the United States in 2015, and 15,000 deaths within 30 days of the initial diagnosis. Clostridium difficile (C. diff) is a common bacterium found in the human intestine, but it becomes a serious gastrointestinal infection when individuals have been exposed to antibiotic therapy; the antibiotics kill off the good gut bacteria, leaving C. diff to flourish. There are significant risk factors associated with getting C. diff: patients who are immunosuppressed, patients who have been on antibiotic therapy, and the elderly population are at an increased risk, though anyone can get a C. diff infection. Symptoms of a C. diff infection are diarrhea, abdominal pain, fever, and fatigue. These symptoms can advance to a complication of a severe inflammation of the colon; pseudomembranous colitis, which can also lead to further complications of toxic megacolon (a severe form of colonic distension). The mode of transmission of C. diff can be either direct (person to person) or indirect (transmission through a contaminated object). It can also be healthcare associated or community acquired. C. diff spores can be transmitted from staff, visitors, and patients by hands or other contaminated surfaces; additionally altered normal intestinal flora caused by antibiotic therapy allows growth of C. diff in the colon. Coming in contact with contaminated surfaces, devices, or material with C. diff spores can easily be transferred to individuals by hands that have touched a contaminated surface or item. Some examples of surfaces, devices, and materials that could be contaminated with C. diff spores in healthcare settings and community/outpatient settings are commodes, bath tubs, showers, hand rails, bed rails, counter tops, door handles, drawer handles, light switches, clothing, medical equipment, blood pressure cuffs, and walking aides.
It is important to use an EPA Registered antimicrobial effective against C. diff to clean and disinfect surfaces, devices, and materials to prevent the spread of C. diff. Also, please keep in mind that alcohol based hand sanitizer is ineffective against C. diff, so hand washing with soap and water is a must when coming into contact with someone who has or potentially has C. diff and their environment. A significant factor contributing to the seriousness of this infection is inappropriate antibiotic treatments (for example, antibiotics used for a viral infection, or antibiotics that aren’t effective against a particular bacteria). Antibiotics cause a disruption in the normal intestinal flora which leads to an overgrowth of C. diff bacteria in the colon. The leading antibiotics known to disrupt the normal intestinal flora include, but are not limited to Ampicillin, Amoxicillin, Cephalosporins, Clindamycin, and the broad spectrum antibiotics. To do your part in preventing the spread of C. diff, you should take antibiotics only as prescribed by your doctor and complete the full course of treatment (don’t stop taking them when you feel better), tell your doctor if you’ve been on antibiotics and you get diarrhea within a few months, wash your hands before eating and after using the restroom, and try to use a separate bathroom from those who have had diarrhea or be sure the bathroom is cleaned well if someone with diarrhea has used it. Preventing infections and improving antibiotic prescribing could save 37,000 lives from drug-resistant infections, and an estimated $3,800,000,000 in medical costs over the course of 5 years. Acute flaccid myelitis (AFM) is a condition that affects the nervous system, specifically the spinal cord. Most people who experience AFM will have limb weakness, but some people also experience facial droop/weakness, difficulty moving the eyes, drooping eyelids, and difficulty swallowing or slurred speech. Numbness or tingling is rare, and some people experience pain in their arms and legs. Severe symptoms include respiratory failure as a result of breathing muscles that become weak. AFM has no specific treatment, but interventions may be ordered by a doctor on a case-by-case basis.
Acute Flaccid Myelitis (AFM) has a variety of causes, but viral infections such as enteroviruses (polio and non-polio), West Nile Virus and those viruses in the same family, herpes viruses, and adenoviruses have been attributed to the cause of AFM. You can prevent AFM by being up to date on all recommended vaccinations, including poliovirus. You can also protect yourself and your family from mosquito borne viruses that can cause AFM by using mosquito repellent and staying indoors at dawn and dusk. Other ways you can protect yourself from causes of AFM are:
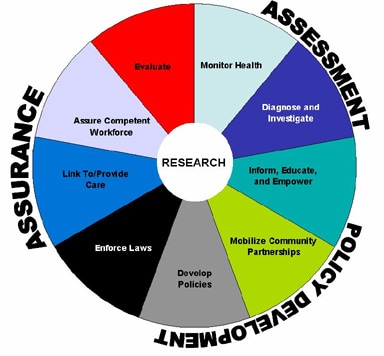
Syndromic surveillance is part of one of the three core public health functions: assessment, policy development and assurance. Assessment entails:
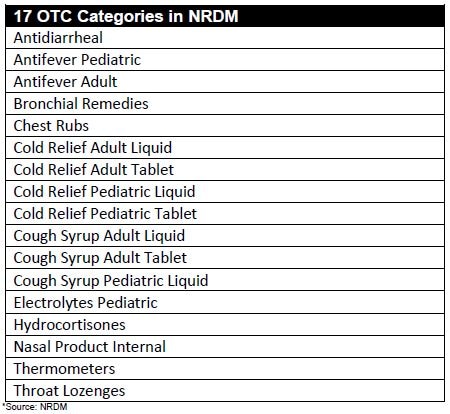
As part of the assessment function, public health officials and practitioners use syndromic surveillance to monitor the health status of a population and make decisions that impact the health of these populations. Syndromic surveillance is special because it is near real-time data, which allows for situational awareness and for decisions to be made based on what is currently happening versus what has happened in the past. A great example of syndromic surveillance in action is when we are able to detect an increase in illness during an event, such as Hot August Nights or the Rib Cook-Off. We may see an increase in hospital or urgent care visits for gastrointestinal illness, which would alert us that the event needs further attention. Syndromic surveillance is a great tool that we have at our disposal to navigate these situations, deploy appropriate resources and implement targeted interventions. At this time, approximately 80% of hospitals and 10% of urgent cares statewide are reporting their data at least daily. Moving forward, Nevada will make a strong push to get more urgent cares on board. Another way we can use syndromic surveillance is through the National Retail Data Monitoring System (NRDM). This system looks at over-the-counter drug sales and alerts us if there is an unexpected increase in the sales of specific medicine categories. Of course, it takes promotional sales into consideration and adjusts for it. Here are the medications NRDM tracks: While this system has great capabilities, it’s important to remember that not every store sends their sales data to NRDM so there are some gaps in coverage.
Syndromic surveillance is a great tool to serve as an early warning system for public health events. While originally developed to detect a large scale release of a biological agent, it has been utilized in many different ways. On the national level it has been used to track things like infectious disease outbreaks and pandemics, mass gatherings, natural and man-made disasters, injuries, chronic conditions and utilization of health care. For more information on the National Syndromic Surveillance Program, see https://www.cdc.gov/nssp/overview.html For more information on Nevada’s Syndromic Surveillance Program, see http://dpbh.nv.gov/Programs/BioSense/Syndromic_Surveillance_-Home/ What is Tuberculosis (TB)? TB is caused by a bacteria called Mycobacterium tuberculosis, which usually attacks the lungs but can attack anywhere in the body including the kidney, spine, and even the brain. One of the most interesting aspects about TB is that not everyone infected becomes sick. There are two manifestations: TB disease and latent TB infection (LTBI). What is the Difference between TB Disease and Latent TB? How is Someone Infected with TB? A person could become infected if they are near someone who has TB Disease and that person is infectious. Sneezing, coughing, laughing, or singing can transmit those TB bacteria into the air and the other person can inhale them. But, here is a list of ways TB cannot be spread:
TB and Travel? TB is much more common in other countries than it is in the United States, so travelers need to be aware of their risk. In fact, TB has become the leading infectious disease worldwide, even surpassing HIV/AIDS. Avoid close contact or prolonged time spent with known TB patients in enclosed areas. If travel will include being in close contact or prolonged time spent with those who are infectious with TB disease, be sure to have a TB skin or blood test administered and read before leaving the US. If the test is negative, have the same type of TB test completed 8-10 weeks after returning to see if you have become infected. Air travel poses a fairly low risk of contracting TB of any kind; especially on short flights under 8 hours. TB in Nevada While this is not a regulation most other states require, Nevada state law mandates that healthcare workers must have a TB test upon hire and annually after that. Nevada also goes the extra mile to do testing on high risk groups like inmates in correctional facilities, refugees, and immigrants. Finally, a new law requires reporting of any child under the age of five who tests positive for LTBI. World TB Day: March 24th This annual event commemorates the date in 1882 when Dr. Robert Koch announced the discovery of TB. The theme of 2017 is “Unite to End TB.” How is Nevada getting involved in World TB Day? An educational project will reach 2,000 providers (pediatricians, infectious disease doctors, and family practice providers among many others) who either work with children or individuals who may have TB Disease or LTBI. The project will include information about World TB Day, a TB screening tool, several CDC and Nevada resources, TB facts and literature, a list of TB related laws, and the reporting form.
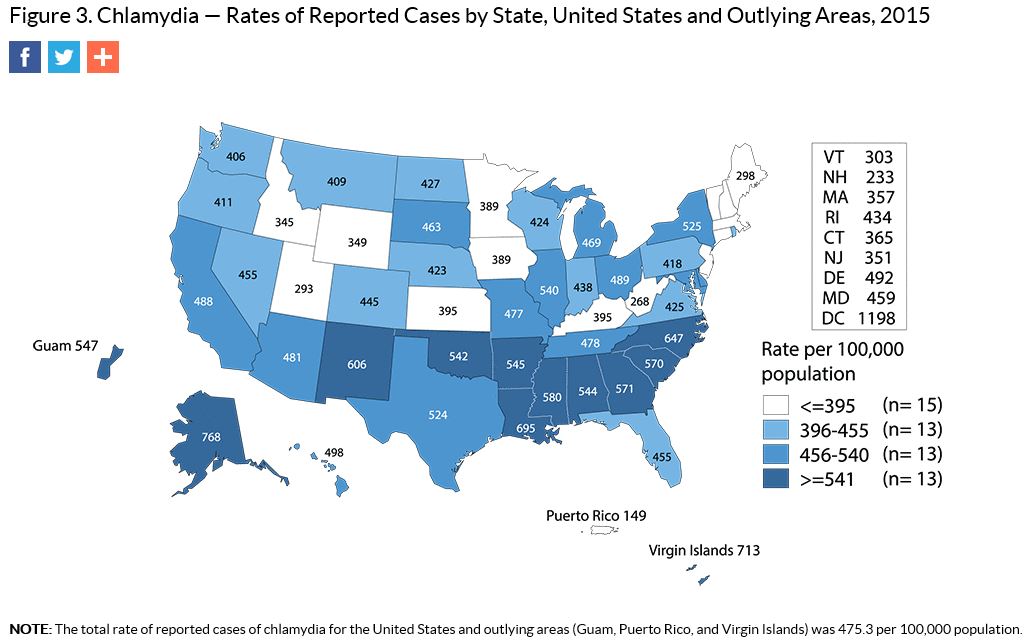
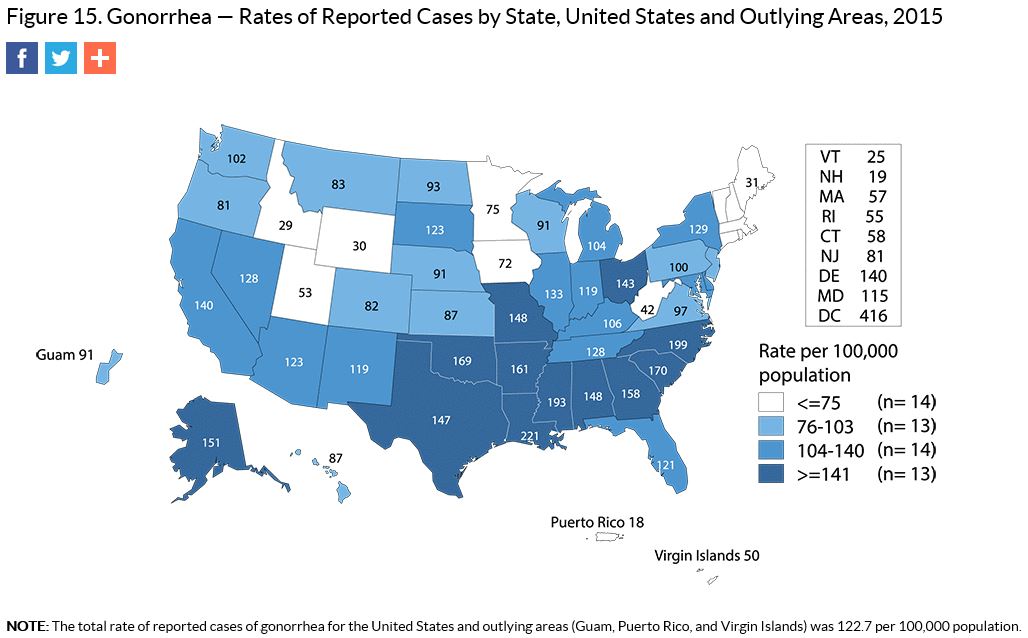
Want to know more about TB in Nevada? Check out OPHIE’s TB page here and be sure to note the resources available on the right side of the main screen. You’ll find resources for the community, the media, and providers, as well as forms, grant information, publications, and upcoming training and education opportunities. Still want more information? Check out CDC’s TB page here. Valentine’s Day is this month, and you know what that means: LOVE is in the air! Something else that’s out and about? Sexually transmitted diseases (STDs). While STDs are a concern year round, now is a great time to remind everyone of their presence. At the national level, STDs (chlamydia, gonorrhea, and syphilis) were at a record high as of 2015. Chlamydia Chlamydia is the most common STD in the United States. It is an easily curable STD that can affect both men and women. Complications from chlamydia are more impactful to women; it can cause permanent damage to the reproductive system, which can make pregnancy difficult or impossible if left untreated. What makes chlamydia tricky is that most people don’t even know they have it since it often has no symptoms. If symptoms do appear, it’s often not until several weeks after infection. In 2015, a total of 1,526,658 chlamydial infections were reported to CDC. That’s 475.3 people per 100,000 in the nation. Nevada came in under the national rate, only slightly better at 455 people per 100,000. Persons ages 15-29 accounted for almost 80% of the chlamydia cases in Nevada. For more information on chlamydia, visit the CDC’s chlamydia page. Gonorrhea Anyone who is sexually active can get gonorrhea, but it is most common in youth and young adults ages 15-24. The infection can cause serious complications if left untreated, but, like chlamydia, it can be treated. Gonorrhea affects men and women differently. Some people with gonorrhea may have no symptoms at all. Men with the infection are sometimes aware of swelling, discharge and a burning sensation. When symptoms arise in women, they are often mild and mistaken for a bladder or vaginal infection. While gonorrhea can be cured with the right treatment, it is becoming harder and harder to treat now that drug-resistant strains are increasing. If your doctor treats you for gonorrhea but you are still experiencing symptoms after a few days, you should return to your provider for follow up. For 2015, the national rate of infection is 122.7 people per 100,000. Nevada’s rates are slightly higher at 128 per 100,000. In Nevada, persons ages 15-34 accounted for 76% of the gonorrhea cases. For more information on gonorrhea, visit the CDC’s gonorrhea page. Syphilis Syphilis is an STD that can cause very serious long-term complication if left untreated. It’s important to know that treatment will not be able to reverse any of the damage already done, so it’s important to seek treatment as early as possible. A syphilis infection can result in many possible symptoms. It’s been called “the great imitator” because it can look like many other diseases. There are four stages of adult syphilis:
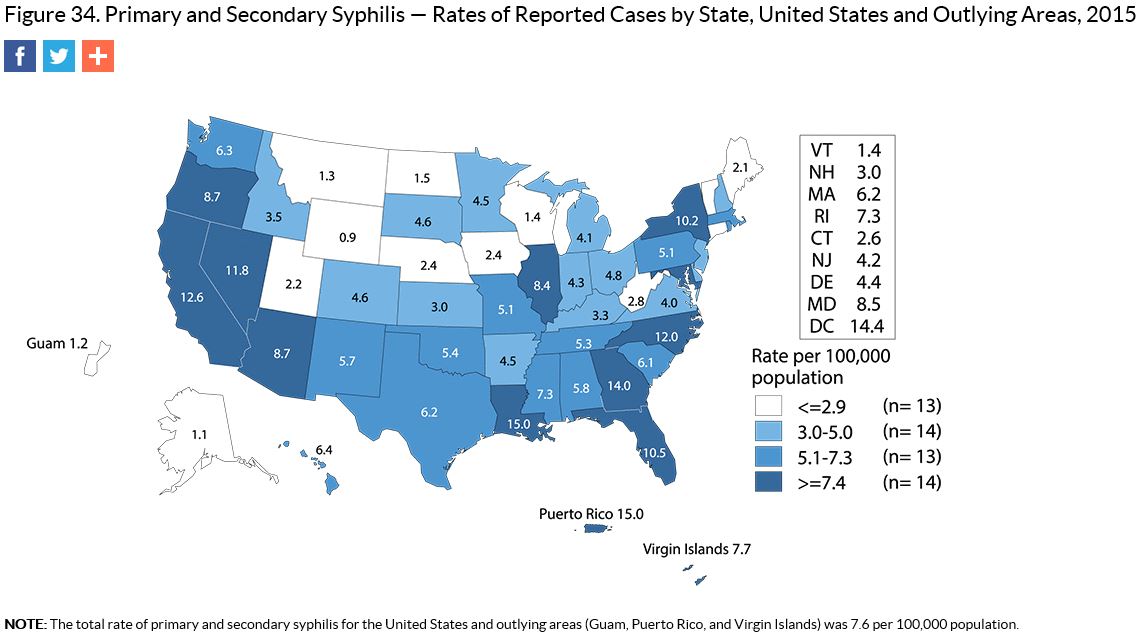
The national rate for syphilis was 7.6 per 100,000 people. Nevada’s rate was much higher, at 11.8 per 100,000. For more information on syphilis, visit the CDC’s syphilis page. Prevention Tips
Check out this great blog from Christian John Lillis, Executive Director of the Peggy Lillis Foundation posted today on the CDC's Safe Healthcare Blog:
I had scarlet fever when I was six years old. The infection had me in the hospital for a week, while the doctors struggled to diagnose my illness and then managed my treatment with antibiotics. One of my earliest memories is being shaken awake at least twice a night by a large, looming nurse to take another oral dose of antibiotics. From the mid-nineteenth century through the Second World War, scarlet fever was a significant cause of childhood death causing upwards of 60,000 deaths at the turn of the century. Though death rates were decreasing throughout the 20th century1, it was the discovery and use of antibiotics that made scarlet fever a manageable illness. Luckily for me, by the time I was diagnosed in 1979, the antibiotic penicillin was widely available. My mother took me home following my week-long stay in the hospital. Though antibiotics likely saved my life, they were also presumed to be responsible for my adult teeth coming in discolored and with overly porous enamel. Every dentist I saw, including the one who eventually helped remove some of the discoloration, blamed the huge doses of antibiotics I was given as child. Despite having otherwise straight and nicely shaped teeth, the discoloration always bothered me. The Story of Peggy Lillis The Other Side of Antibiotics Unlike a lot of Americans, I’ve rarely used antibiotics throughout my life. While in high school and college, I tended to get strep throat at least once every winter. The doctor would always prescribe antibiotics and I would never take them. Instead, being a “young invulnerable,” I felt I could fight it off myself. I would gargle with warm salt water, drink tea, and live on cherry cough drops. I was never sick for more than 10 days and by the time I was 25, the bouts of strep stopped. Thankfully, I did not have any complications from strep throat and remained healthy in my 20s and 30s. But truthfully, I rarely thought about antibiotic use. That changed with the death of my mother Peggy Lillis on April 21, 2010 from a Clostridium difficile infection. Like so many other Americans, my mother’s deadly C. diff infection began with her being prescribed a prophylactic dose of an antibiotic, clindamycin, following a root canal. Within four days, she began to experience diarrhea. Ten days after beginning her course of antibiotics, she was dead. Prior to my mother’s death, I would never have imagined that an antibiotic could precipitate a deadly disease. Like many Americans we had never heard of Clostridium difficile. Nor did we realize the system-wide effects that many antibiotics have on the body. I’ve wondered since Mom’s death if knowing how antibiotics had affected my teeth made me subconsciously reticent to take them. In our mother’s memory, my brother Liam and I founded the Peggy Lillis Foundation (PLF) to raise C. diff awareness and advocate for policy changes to combat the disease. A key element of our work is educating the public about the judicious use of antibiotics. To that end, we team up with organizations like the Centers for Disease Control and Prevention (CDC) to share stories like our mother’s, provide the patient and caregiver perspective, and develop shared goals and strategies. Throughout this year, we’ve been working with CDC and other organizations to raise awareness of the role of antibiotics in causing C. diff infections. Examples include:
For this year’s Get Smart About Antibiotics Week, we worked with CDC on a new video about our mother’s story. The video clearly demonstrates that antibiotic use can lead to real harm, even death. I am living proof that antibiotics are incredibly important and vital drugs. At the same time, my mother would likely still be alive today if she’d never taken that course of clindamycin. Antibiotics can save lives. But antibiotics can take lives too. The difference in our two outcomes demonstrates how desperately we need to be smarter about antibiotics. 1 Smallman-Raynor, Andrew Cliff, Peter Haggett, Matthew (2004). World Atlas of Epidemic Diseases. London: Hodder Education. p. 76. ISBN 9781444114195. Check out the blog and more information here. |
AuthorOPHIE records and analyzes data from disease investigations, identifies risk factors, and provides education on disease prevention in Nevada. Archives
November 2018
Categories |








 RSS Feed
RSS Feed
